Blog > Male Menopause Is Not Just for Older Men
Male Menopause Is Not Just for Older Men

Depression, loss of sexual desire, erectile dysfunction, and various physical and emotional symptoms can manifest in certain men during their late 40s to early 50s. This phenomenon is described as male menopause or andropause (androgen deficiency in the aging male). It is not solely an issue that affects older men, as even younger men can experience low testosterone levels. The decline in testosterone is not exclusively linked to aging. Numerous factors, including stress, mood, diet, overall health, medications, being overweight, and inadequate sleep, can influence the level of this hormone.
Understanding andropause

The term “male menopause” has been used to explain the decline in testosterone levels that occurs with aging. However, it is important to note that the hormonal changes associated with aging differ between women and men.
In women, the cessation of ovulation and the subsequent significant decrease in hormone production takes place within a relatively short period of time, which is commonly referred to as menopause. Conversely, in men, the decline in testosterone and other hormone production happens gradually over the course of many years, and the exact implications of this decline are not evidently clear.
Androgen deficiency occurs when the body produces lower quantities of male sex hormone, particularly testosterone, than what is necessary for maintaining good health. This insufficiency can stem from complications in the brain regions that govern testicular function (the pituitary gland and hypothalamus), or from issues within the testes themselves. Although a gradual and modest decline in sex hormone levels is observed in male populations starting around the age of 30, not all men encounter this decline. In most cases, the decrease in testosterone levels appears to be associated with the onset of other medical conditions.
Symptoms of low testosterone

Symptoms associated with low testosterone include:
- Hot flushes or sweats
- Prolonged fatigue and reduced energy levels
- Diminished muscle mass and weakened physical strength
- Male breast discomfort or swelling
- Increased accumulation of body fat, particularly around the abdomen
- Mood fluctuations, including irritability or depression
- Decreased libido and sexual dysfunction
- Loss of bone density and heightened risk of fractures
- Impaired cognitive function and difficulties in concentration
Factors responsible for andropause

Many of the above symptoms in younger men can be attributed to lifestyle factors or psychological issues. Stress, depression, and anxiety, for instance, can result in erectile dysfunction, low sex drive, and mood swings.
In addition to psychological causes, there are also physical factors like smoking or alcohol abuse which can contribute to low levels of testosterone.
Psychological problems often arise from work or relationship difficulties, financial troubles, or concerns about aging parents.
Another factor that can play a role in andropause is “midlife crisis,” which occurs when men believe they have reached the halfway point in life. Worries about achievements in their career or personal life can lead to a period of depression.
In certain instances, the symptoms associated with the “male menopause” may be attributed to hypogonadism, a condition where the testes produce insufficient or no hormones.
In some, hypogonadism can be present from birth, leading to symptoms such as delayed puberty and small testes.
Additionally, hypogonadism can occasionally develop later in life, particularly in men who are obese or have type 2 diabetes. This condition is referred to as late-onset hypogonadism and can give rise to symptoms resembling the “male menopause.” However, it is important to note that this is an uncommon and specific medical condition that is not a natural part of the aging process.
Diagnosis of androgen deficiency
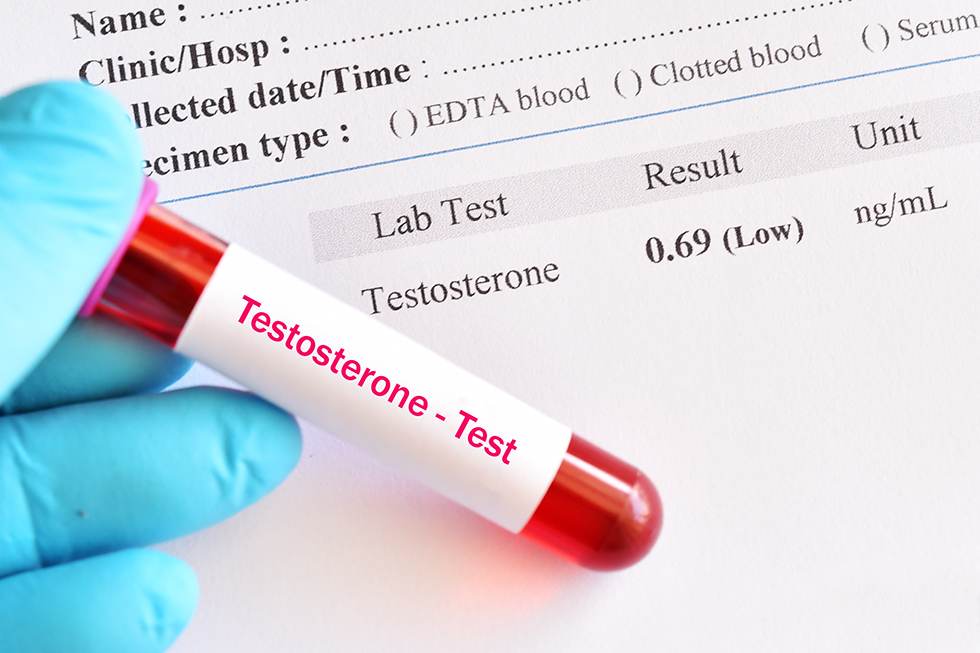
The diagnosis of androgen deficiency involves several assessments such as:
Medical history: A comprehensive medical history is obtained, encompassing information on fertility, sexual function, signs of androgen deficiency, any other existing medical conditions, occupation, as well as prescribed and non-prescribed medications and drug usage.
Physical examination: During the physical examination, a comprehensive general check-up is conducted, which includes assessing the testicles’ size and examining for any signs of breast development.
Blood tests: To determine the amount of testosterone in the blood, blood tests are performed. For optimal accuracy, it is best to have a fasting blood test in the morning when the body produces the highest levels of testosterone. It is recommended to measure testosterone levels on two separate mornings to obtain reliable results. It is also essential to measure the levels of pituitary hormones.
Other tests: In order to determine the cause of testosterone deficiency, additional tests may be necessary. These tests might involve conducting genetic tests to diagnose genetic conditions like Klinefelter’s syndrome or performing MRI scans of the brain to examine the pituitary gland. Moreover, semen analysis can help evaluate the fertility potential of men with androgen deficiency.
Treatment for androgen deficiency
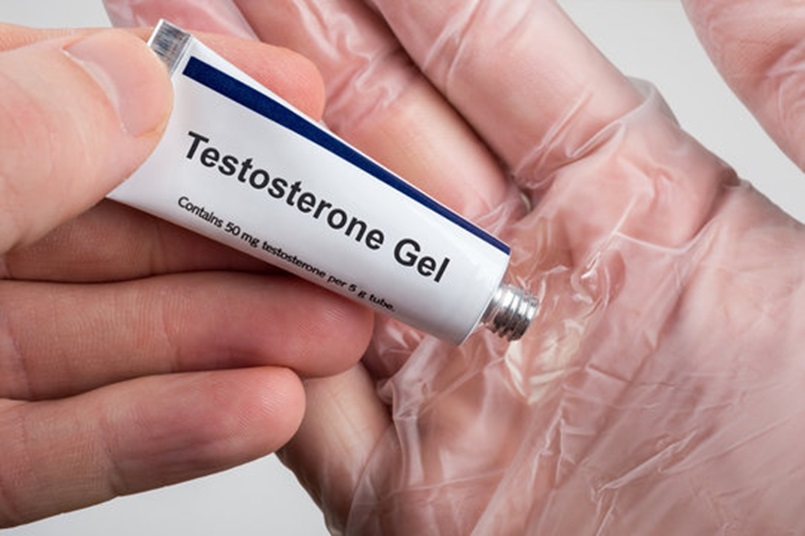
Doctors will provide guidance on how to modify one’s lifestyle in order to alleviate stress, maintain a healthy diet, ensure sufficient sleep, engage in regular exercise, limit alcohol consumption, and quit smoking. If the symptoms continue despite these general measures, the doctor may consider hormone replacement therapy.
Treatment for confirmed androgen deficiency is primarily based on the administration of testosterone replacement therapy. The most effective methods of delivering testosterone include skin gels, creams, or injections (either short-acting or long-acting). In cases where the deficiency is caused by issues with the pituitary gland and the individual desires to father a child, the doctor may suggest gonadotrophin injections multiple times a week for several months.
This treatment aims to stimulate both testosterone and sperm production. However, it is important to note that testosterone therapy is not recommended for men who are actively trying to help their partner conceive, as it acts as a potent contraceptive by suppressing the pituitary hormones responsible for sperm production.
If individuals are experiencing androgen deficiency and are attempting to conceive with their partner, it is advisable to consult a fertility specialist.
Regular check-ups with a doctor are necessary if they are undergoing testosterone replacement therapy. The frequency of these appointments will depend on factors such as age and other risk factors for prostate cancer.
Before initiating testosterone replacement therapy, older men should undergo screening for prostate cancer, as elevated testosterone levels could potentially promote the growth of undetected cancer cells.
Andropause, also known as “male menopause,” occurs when there is a decline in the production of testosterone in men aged between 40-60. Low testosterone levels in younger males is typically associated with stress, alcohol consumption, certain medications, obesity, and infections. Hormone replacement therapy is a potential treatment option for this condition.
For those men facing androgen deficiency, AndroNeo, in Bangalore offers advanced solutions. With a team of specialized professionals in reproductive health, they ensure exceptional care for managing sensitive cases. If you are dealing with andropause, consult the specialists at AndroNeo.
Recent Post
- Penile Implant Surgery: A Permanent Solution to Erectile Dysfunction from the expert Andrologist in Bangalore
- Testosterone – why is it so important
- Bengaluru’s Leading Expert in Andrology (Male Fertility and Sexual Health) and Prosthetic Urology – Dr Pramod Krishnappa
- Varicocele – The Hidden Cause of Male Infertility
- No Sperm and Its Link to Genetic Factors: An Exploratory Guide
Related Post
Penile Implant Surgery: A Permanent Solution to Erectile Dysfunction from the expert Andrologist in Bangalore
Penile Implant Surgery: A Permanent Solution to Erectile Dysfunction from the expert Andrologist in Bangalore Living with erectile dysfunction (ED) is not only a physical
Testosterone – why is it so important
Testosterone – why is it so important Testosterone hormone is one of the most important hormones in our body, it is primarily a male hormone
Bengaluru’s Leading Expert in Andrology (Male Fertility and Sexual Health) and Prosthetic Urology – Dr Pramod Krishnappa
Bengaluru’s Leading Expert in Andrology (Male Fertility and Sexual Health) and Prosthetic Urology – Dr Pramod Krishnappa Overview Dr. Pramod Krishnappa is an exceptional Andrology
Varicocele – The Hidden Cause of Male Infertility
Varicocele_ The Hidden Cause of Male Infertility Infertility in men is a problem for millions of couples around the world, and one of the common
No Sperm and Its Link to Genetic Factors: An Exploratory Guide
No Sperm and Its Link to Genetic Factors: An Exploratory Guide Azoospermia, a leading cause of male infertility, occurs when a man’s ejaculate (semen) does
Penile Implant For Erectile Dysfunction: Preparation, During & After Surgery
Penile Implant For Erectile Dysfunction: Preparation, During & After Surgery A penile implant, also called a penile prosthesis, is a treatment method used to treat
Author: Dr. Pramod Krishnappa
